Publications
Category:

The SRHR Spotlight Newsletter
Hello reader,
Welcome back to the SRHR Spotlight Newsletter! Dive into a world of curated insights, thought-provoking discussions, and fresh perspectives with our tales.
Whether you’re a seasoned enthusiast or just starting your journey into our niche, we’ve got something special for you.
Enjoy your reading.
Reproductive Health Uganda

The SRHR Spotlight – October 2023

RHU Annual Report, 2022

Uganda Launches the FP2030 commitments
On the 3rd November, Uganda launched the FP2030 commitments. The objective of the launch was to create awareness, understanding and momentum leading to the global launch that is due November 18th 2021. Uganda has made several commitments towards the FP 2030 to address the gaps in ensuring access to family planning commodities.
Reproductive health Uganda alongside other civil society organizations will partner with the Ministry of Health to see the commitments to fruition.
Speaking at the launch, the minister of Health Dr. Jane Ruth Aceng underlined that Government is keen on implementing its commitments on family planning. She said the focus should now change to the boy child.
Speaking at the launch of the Uganda Family Planning 2030 Commitments in Kampala on Wednesday, Aceng said boys ‘need to know the dangers of making a teenage girl pregnant’. ‘The focus has been on the recipient of the pregnancy and not the giver.’
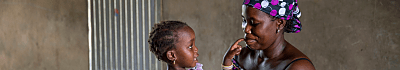
Over the past nine years, governments, civil society, multilateral organizations, donors, the private sector and the research community, have come together around an ambitious goal: to enable 120 million additional women and girls to use modern contraception by 2020. Working together in partnership, much has been achieved, but more remains to be done.
The global family planning community agreed that the gains of the last nine years should be sustained by extending this pivotal partnership. Through a global consultation, stakeholders from around the world provided their input on the future of family planning. Together, the community created a shared vision for 2030 that builds on progress achieved to date, adapts the partnership in response to the lessons of the first nine years and positions us to achieve the future women and girls around the world are asking for.
The collective feedback has formed the basis of a vision, guiding principles, and focus areas. With this foundation, and informed by the family planning community consultation, the new partnership will be built over the course of 2021.
The Uganda Family Planning 2030 Commitments include the following:
– to increase equitable access and voluntary use of modern contraceptive methods for all women and couples
– to increase funding for adolescent sexual and reproductive health programmes
– to ensure contraceptive commodity security
– to strengthen the policy and enabling environment for family planning
– to strengthen the policy and enabling environment for family planning
– to strengthen family planning data use at all levels
– to address family planning myths and misconceptions through evidence-based sexual and behavioral change communication and advocacy
Guiding Principles of the commitments
- Voluntary, person-centered, rights-based approaches, with equity at the core: This guiding principle reflects the fundamental belief that individuals should be able to freely make choices that reflect their desires and needs. Every decision, action, and investment made by the partnership will reflect this belief – that each person has the same right to quality family planning, regardless of their geography, socioeconomic status, gender, or culture.
- Empowering women and girls and engaging men, boys, and communities: Positive male inclusion is needed to truly transform normalization of family planning and at the same time share the burden of the decisions and implications of family planning. This must happen in tandem with empowerment of women and girls to create true equity.
- Building intentional and equitable partnerships with adolescents, youth, and marginalized populations to meet their needs, including for accurate and disaggregated data collection and use: These populations have been consistently underserved, so the partnership commits to prioritizing them in all future work.
- Country-led global partnerships, with shared learning and mutual accountability for commitments and results: Country commitments drive progress with support from regional and global stakeholders for implementation, coordination, and accountability.

No schools, no blood: How Covid-19 closure has worsened shortage
No schools, no blood: How Covid-19 closure has worsened shortage
Written by BY GILLIAN NANTUME – September 7th, Daily Monitor , Uganda
Reproductive Health Uganda through the SET SRHR project is advocating for increased funding to the National blood bank. This is through a campaign dabbed Saving lives through greater investment in safe blood transfusion services. Join the conversation on social media using #SupportTheUGBloodBank #SaveLives #WeAreRHU
Blood transfusions are a strong pillar in modern medicine and they have saved the lives of countless people. Women with pregnancy related complications, need donated blood more than all other groups, except children below the age of five. Dr Elizabeth Nabiwemba, the project director of SET-SRHR, says blood loss mainly affects women in childbirth because their blood levels are already low due to the pregnancy.
Who is at risk
“Haemorrhage is the number one killer of pregnant women. When there is no blood in a hospital the risk of a woman dying in labour is very high. She does not have to lose much blood to die.”
Sarah Mutegombwa, the programme manager for blood donor recruitment at Uganda Red Cross Society (URCS) says most of the donated blood goes to children below five years.
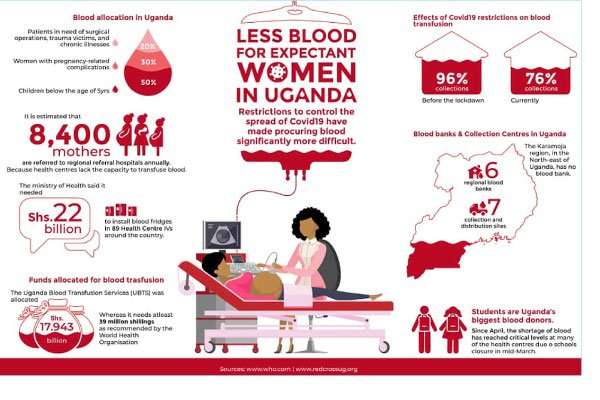
“These children take at least 50 percent of the blood because they become anaemic when they suffer from severe malaria and malnutrition. Women with pregnancy-related complications take up 30 percent of the demand, while the remaining 20 percent is shared by those in need of surgical operations, trauma victims, and those who suffer from chronic illnesses, such as cancer and sickle cell disease.”
Mutegombwa adds that one unit of blood can serve three children, because they use only one or two components of the blood, such as red blood cells, platelets, or the plasma. An adult, though, can consume as many whole units of blood as the need arises. In contrast, in high-income countries about 76 percent of the donated blood is received by patient groups over the age of 65.
Before the COVID-19 pandemic dominated the focus of health policymakers, the Ministry of Health (MoH) had, in its 2020/21 budget, said it would target equipping Level IV Health Centres to provide blood transfusion services in order to improve reproductive, maternal, neonatal, child and adolescent health services.
According to the Health Ministerial Policy Statement for the Financial Year 2020/2021, it is estimated that 8,400 mothers are referred to regional referral hospitals annually because Level IV Health Centres lack the capacity to perform obstetric care as they cannot transfuse blood. The ministry said it needed Shs2.2 Bn to install blood fridges in 89 Level IV Health Centres around the country.
Chronic blood shortages worsened
There are seven blood collection and distribution sites located in the districts of Lira, Nebbi, Jinja, Masaka, Kampala, and Hoima. The collections sites are not fully-fledged blood banks because they do not have testing facilities. Restrictions to control the spread of the coronavirus have made procuring blood, even from these few points, significantly more difficult.
While anyone between 17- 60 years can donate blood as long as they are in good health, students are Uganda’s biggest blood donors.
“During the school term, we run continuous blood donation mobilisations to replenish what is in the blood banks, until the students get holidays. As a country, we have been getting 70 percent of our total blood donations from schools. The remaining 30 per cent is collected from the community. Some areas organise and then, call us, with the intention of donating blood,” Mutegombwa says.
She adds that in schools, more boys donate blood than girls. “For girls, the barriers to donating are many. For instance, she cannot donate blood if she has recently completed her period because she has lost blood. Also, in the communities, there are restrictions on a pregnant woman and breastfeeding mother donating blood.
However, when in terms of the HIV prevalence rate, we target low risk donors, where the rate of infection is too small. Before we go to a community, we screen its prevalence levels and also give community members information so they can self-exclude themselves.”
Blood has a shelf life of 35 days. Schools were closed in mid-March. Since April, the shortage of blood has reached critical levels at many of the health centres. This shortage gives unscrupulous health workers an opportunity to raise the price of the few units of blood available.
“During the holidays, we would shift the blood donation mobilisation drives to the communities. But, the pandemic broke out during the school term, so we had to quickly switch to the communities. Unfortunately, we ended up with a [total] lockdown,” Mutegombwa says.
Who has been donating?
With the broader lockdown came bans on public gatherings and public and private transport. URCS switched to soliciting for blood from individual registered donors.
Uganda has between 80,000 and 90,000 registered blood donors, most of who donate twice a year. Mutegombwa says: “We would call a donor, pick them from home and drive them to our offices. After the donation, we took them back home.
Sometimes, we spent one hour on transporting a donor. On average, we would pick up between 20 to 30 donors per day. Each of these can only donate one unit of blood every three months if they are male or every four months if they are female.”
Cost of blood supply
The government meets the costs of blood donation. But sometimes, especially during the lockdown, groups such as the Indian Association, offered to transport blood donors.
Although both public and private transport are operational, blood donations are still low due to the restrictions on public gatherings in communities, and also, due to the fact that schools are still closed. Mutegombwa says prior to Covid19, their outreach teams would hold at least 30-40 minute-long awareness campaigns in a month, targeting at least 100 people but now it is difficult to organise more than 20 people in one place.
The bleeding processes (drawing blood from a donor) also takes much longer. Previously, one nurse could tend to two donors at the same time. Now, due to the physical distancing and other Covid19 related regulations, a nurse will spend about 15 minutes bleeding one person.
Dr Mathias Lugolobi is District Health Officer in Wakiso. He says, “We have four government and eight church-based facilities that can perform blood transfusions. Ideally, each facility needs 30 blood units per month.”
However, they never get that many units and Lugoloobi adds that during the lockdown the blood supply dwindled to the bare minimum. When there are shortages of blood, smaller health centres outside the main urban areas are de-prioritised.
Dr Francis Kakooza, the Kayunga District Health Officer is also in charge of its general hospital. He says his hospital gets only about 15 to 20 units a week yet, ideally, they need 30 to 40 units. In times of shortages they do not get any blood from Nakasero blood bank.
“At times, we only get 10 units. So, we transfer patients who need blood to Jinja or Kampala districts. However, at the peak of the lockdown, we only made referrals to Kampala because in most cases, Jinja also suffered blood shortages. Right now, we are renovating the hospital and soon we will have an emergency trauma unit. This means we will need more blood,” he says.
The WHO standard
The Uganda Blood Transfusion Services (UBTS), the institution mandated to collect, test, store and distribute blood was allocated Shs17.824 billion (USD 4.8 million) in the 2020/2021 Financial Year. Of this amount, Shs 4.9 billion will go to wages and salaries, Shs 4.758 billion on travel and transport, Shs 2.675billion on general expenses, Shs 1.479billion on maintenance, and only Shs 476 million on supplies and services.
According to the World Health Organisation’s Global Database on Blood Safety, a country should be able to collect blood equivalent to one percent of its population. Uganda has an estimated population of 45,903,545 people.
This means the country needs to collect 459,035 units of blood annually. According to URCS, it costs USD85 (Shs 331,500) to collect one unit of blood. This means UBTS needs USD 39 million (Shs152.1 billion) if it were to meet the WHO recommendations. Mutegombwa says that the country is not set to meet the WHO target at the moment.
“Instead of the 459,035 units of blood, our target is 300,000 units a year,” she says.
That target, which translates into 25,000 units a month, is also often missed. By the end of last year, only 288,000 units had been collected,” she says.
Coronavirus restrictions made a bad situation worse. “Before the lockdown, as a country, we were at 96 percent collections. Currently, we are at 76 per cent. In April, only 14,768 units were collected, 23,032 units were collected in May and 19,050 units in June,” Mutegombwa adds.
Blood donation drive
The blood shortage has motivated medical doctors to fundraise for blood. Dr Joseph Gavin Nyanzi, the in-charge of Cherish Health Centre, a private-not- for-profit facility in Garuga, Wakiso district, has partnered with the Rotary Blood Bank at Mengo Hospital in a donation drive. Dr Nyanzi is also the public relations officer of the Uganda Medical Association.
“Over time, I have realised the need of blood as a medical product. So, on July 31, to commemorate my mother’s 70th birthday, I started a drive. My target is to collect 140 units of blood by September 3, when the drive will end. As of today (August 16) we have collected 20 units. Everyone is welcome to donate blood from Monday to Friday at the Rotary Blood Bank,” he says.
This is the second time Dr Nyanzi is carrying out a . In January last year, his drive had a target of 105 units but he managed to collect 16 units.
“There is only one factory of blood – you and I. If you donate blood, you also get the satisfaction of knowing your blood can make the different between life and death for someone,” he says.
Charting a way forward
On July 16, 2020, the UBTS appeared before Parliament’s health committee and requested for Shs20.5 billion to mitigate the blood shortage. Of this amount, Shs 10 billion wasww to offset a previous debt while the remaining Shs 10 billion was to help UBTS in the current crisis. The money has not yet been received.
However, there is a general feeling that UBTS is getting a lot of money but the problem is with prioritising how the money should be used. With prioritising blood collection, testing and distributing, the Ministry of Finance can be convinced when it comes to the supplementary budget. But the problem isn’t always financial. Mutegombwa says the majority of the registered donors are students.
“Adults fear donating blood because they do not want to know their HIV status. Some believe their blood supply will dwindle if they donate. Lack of information, discouraging cultural and religious beliefs about blood donation is also a hindrance. People see blood donation as taboo. They associate it with human sacrifice!” Mutegombwa says. Dr Nabiwemba says the general community should be mobilised.
“I know a woman who went to her church and talked to the congregants about the blood shortage. She asked them to bring other friends to donate blood in two weeks’ time and it was a successful donation. I think we can do this even in this era of social distancing. We can donate while observing the standard operating procedures.”
According to a Memorandum of Understanding signed between the Ministry of Health and URCS and UBTS, the two organisations are working with village health teams to register potential donors in rural areas.
To engage the public, the URSC has developed the Blood for Uganda App for both android and iOS which people can download and get to know the blood donation sites near them.
Mutegombwa says 114 donors have so far registered with the App. “When there is a need for blood from rare blood types, we activate the contacts in the App and they come to our offices to donate because most of them are walk-in donors.”
The app also creates a database of volunteers who can be reached in time of need and to achieve the No shortage of Blood goal. However, the App can only apply to people who use smartphones. Those who do not have them, have to rely on the honesty of medical workers.

Tips for working from home successfully
Following the outbreak of the Novel Corona virus world wide, most of us have been forced to work from home. We have come up with a few tips to help you work efficiently and effectively from home. Click here to learn more RHU-ICT-COVID-19 WFH

Not ready to get pregnant yet? Here are a few things you could do
These are very unprecedented times. We are no longer dealing with the same challenges as we were before. Times where we knew how not to spread HIV/AIDS or at least contain it. We could easily treat or prevent Sexually Transmitted Infections and disease (STDs/STIs). And now? Chlamydia, Gonorrhoea, Syphilis and even THE HIV/AIDs itself are no match for the Novel Corona virus.
These are indeed very uncertain times, with governments all over the world taking drastic measures to lock down, restrict movements and yet with diminutive hope or certainty that things will go back to normal soon.
Take caution :
With most people working from home or on forced leave and movement restrictions, loneliness, boredom with the so much time is paramount. For those staying with their partners the idea of sex must be flaunting. I mean ‘things’ are freely available on full time basis right?
Please note: Even if you are under self or institutional quarantine, having unprotected sex will still expose you to STIs and STDs and unplanned pregnancies.
But since abstinence is a complicated subject even without the CORONA virus, how can one enjoy their things without fear of getting pregnant or contracting STDS or STIs?
How do i not get pregnant?
Using contraceptives allows people to attain their desired number of children and determine the spacing of pregnancies. They are also very helpful in times such as these where one wouldn’t want to get pregnant.
There are however two methods one can use to delay pregnancy; Traditional and modern methods these are broken down below;
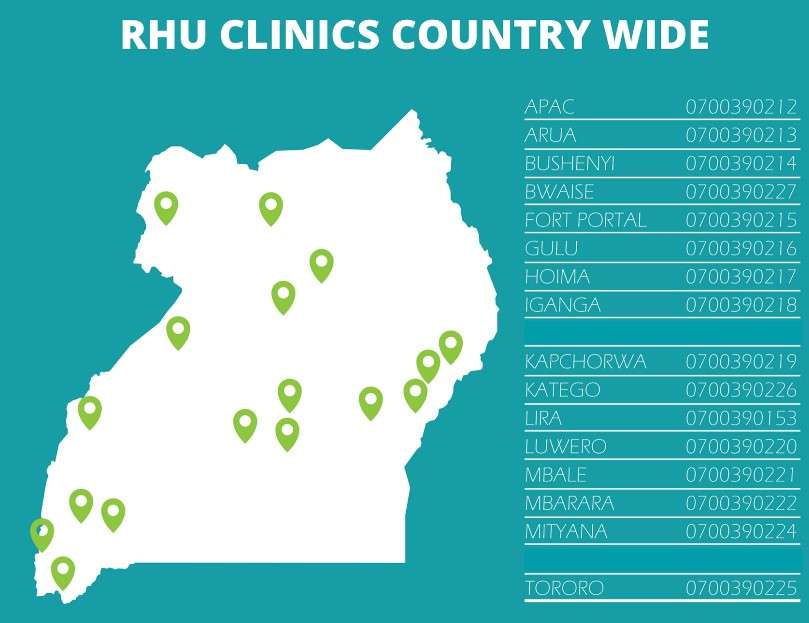
Reproductive Health Uganda clinics remain open across the country You can call any of the clinics in charges for appointments and or questions
What are the Modern methods?
PS: We recommend using modern methods because of their accuracy. They can easily be relied on without fear. These methods are available at any of the Reproductive Health Clinics countrywide. Give us a call to make an appointment
| Method | Description | How it works | Effectiveness to prevent pregnancy | Comments | |
| Combined oral contraceptives (COCs) or “the pill” | Contains two hormones (estrogen and progestogen) | Prevents the release of eggs from the ovaries (ovulation) | >99% with correct and consistent use | Reduces risk of endometrial and ovarian cancer | |
| 92% as commonly used | |||||
| Progestogen-only pills (POPs) or “the minipill” | Contains only progestogen hormone, not estrogen | Thickens cervical mucous to block sperm and egg from meeting and prevents ovulation | 99% with correct and consistent use | Can be used while breastfeeding; must be taken at the same time each day | |
| 90–97% as commonly used | |||||
| Implants | Small, flexible rods or capsules placed under the skin of the upper arm; contains progestogen hormone only | Thickens cervical mucous to block sperm and egg from meeting and prevents ovulation | >99% | Health-care provider must insert and remove; can be used for 3–5 years depending on implant; irregular vaginal bleeding common but not harmful | |
| Progestogen only injectables | Injected into the muscle or under the skin every 2 or 3 months, depending on product | Thickens cervical mucous to block sperm and egg from meeting and prevents ovulation | >99% with correct and consistent use | Delayed return to fertility (about 1–4 months on the average) after use; irregular vaginal bleeding common, but not harmful | |
| 97% as commonly used | |||||
| Monthly injectables or combined injectable contraceptives (CIC) | Injected monthly into the muscle, contains estrogen and progestogen | Prevents the release of eggs from the ovaries (ovulation) | >99% with correct and consistent use | Irregular vaginal bleeding common, but not harmful | |
| 97% as commonly used | |||||
| Combined contraceptive patch and combined contraceptive vaginal ring (CVR) | Continuously releases 2 hormones – a progestin and an estrogen- directly through the skin (patch) or from the ring. | Prevents the release of eggs from the ovaries (ovulation) | The patch and the CVR are new and research on effectiveness is limited. Effectiveness studies report that it may be more effective than the COCs, both as commonly and consistent or correct use. | The Patch and the CVR provide a comparable safety and pharmacokinetic profile to COCs with similar hormone formulations. | |
| Intrauterine device (IUD): copper containing | Small flexible plastic device containing copper sleeves or wire that is inserted into the uterus | Copper component damages sperm and prevents it from meeting the egg | >99% | Longer and heavier periods during first months of use are common but not harmful; can also be used as emergency contraception | |
| Intrauterine device (IUD) levonorgestrel | A T-shaped plastic device inserted into the uterus that steadily releases small amounts of levonorgestrel each day | Thickens cervical mucous to block sperm and egg from meeting | >99% | Decreases amount of blood lost with menstruation over time; Reduces menstrual cramps and symptoms of endometriosis; amenorrhea (no menstrual bleeding) in a group of users | |
| Male condoms | Sheaths or coverings that fit over a man’s erect penis | Forms a barrier to prevent sperm and egg from meeting | 98% with correct and consistent use | Also protects against sexually transmitted infections, including HIV | |
| 85% as commonly used | |||||
| Female condoms | Sheaths, or linings, that fit loosely inside a woman’s vagina, made of thin, transparent, soft plastic film | Forms a barrier to prevent sperm and egg from meeting | 90% with correct and consistent use | Also protects against sexually transmitted infections, including HIV | |
| 79% as commonly used | |||||
| Male sterilization (vasectomy) | Permanent contraception to block or cut the vas deferens tubes that carry sperm from the testicles | Keeps sperm out of ejaculated semen | >99% after 3 months semen evaluation | 3 months delay in taking effect while stored sperm is still present; does not affect male sexual performance; voluntary and informed choice is essential | |
| 97–98% with no semen evaluation | |||||
| Female sterilization (tubal ligation) | Permanent contraception to block or cut the fallopian tubes | Eggs are blocked from meeting sperm | >99% | Voluntary and informed choice is essential | |
| Lactational amenorrhea method (LAM) | Temporary contraception for new mothers whose monthly bleeding has not returned; requires exclusive or full breastfeeding day and night of an infant less than 6 months old | Prevents the release of eggs from the ovaries (ovulation) | 99% with correct and consistent use | A temporary family planning method based on the natural effect of breastfeeding on fertility | |
| 98% as commonly used | |||||
| Emergency contraception pills (ulipristal acetate 30 mg or levonorgestrel 1.5 mg) | Pills taken to prevent pregnancy up to 5 days after unprotected sex | Delays ovulation | If all 100 women used progestin-only emergency contraception, one would likely become pregnant. | Does not disrupt an already existing pregnancy | |
| Standard Days Method or SDM | Women track their fertile periods (usually days 8 to 19 of each 26 to 32 day cycle) using cycle beads or other aids | Prevents pregnancy by avoiding unprotected vaginal sex during most fertile days. | 95% with consistent and correct use. | Can be used to identify fertile days by both women who want to become pregnant and women who want to avoid pregnancy. Correct, consistent use requires partner cooperation. | |
| 88% with common use (Arevalo et al 2002) | |||||
| Basal Body Temperature (BBT) Method | Woman takes her body temperature at the same time each morning before getting out of bed observing for an increase of 0.2 to 0.5 degrees C. | Prevents pregnancy by avoiding unprotected vaginal sex during fertile days | 99% effective with correct and consistent use. | If the BBT has risen and has stayed higher for 3 full days, ovulation has occurred and the fertile period has passed. Sex can resume on the 4th day until her next monthly bleeding. | |
| 75% with typical use of FABM (Trussell, 2009) | |||||
| Two Day Method | Women track their fertile periods by observing presence of cervical mucus (if any type color or consistency) | Prevents pregnancy by avoiding unprotected vaginal sex during most fertile days, | 96% with correct and consistent use. | Difficult to use if a woman has a vaginal infection or another condition that changes cervical mucus. Unprotected coitus may be resumed after 2 consecutive dry days (or without secretions) | |
| 86% with typical or common use. (Arevalo, 2004) | |||||
| Sympto-thermal Method | Women track their fertile periods by observing changes in the cervical mucus (clear texture) , body temperature (slight increase) and consistency of the cervix (softening). | Prevents pregnancy by avoiding unprotected vaginal sex during most fertile | 98% with correct and consistent use. | May have to be used with caution after an abortion, around menarche or menopause, and in conditions which may increase body temperature. | |
| Reported 98% with typical use (Manhart et al, 2013) | |||||
Traditional methods
| Traditional Method | Description | How it works | Effectiveness to prevent pregnancy | Comments | |
| Calendar method or rhythm method | Women monitor their pattern of menstrual cycle over 6 months, subtracts 18 from shortest cycle length (estimated 1st fertile day) and subtracts 11 from longest cycle length (estimated last fertile day) | The couple prevents pregnancy by avoiding unprotected vaginal sex during the 1st and last estimated fertile days, by abstaining or using a condom. | 91% with correct and consistent use. | May need to delay or use with caution when using drugs (such as anxiolytics, antidepressants, NSAIDS, or certain antibiotics) which may affect timing of ovulation. | |
| 75% with common use | |||||
| Withdrawal (coitus interruptus) | Man withdraws his penis from his partner’s vagina, and ejaculates outside the vagina, keeping semen away from her external genitalia | Tries to keep sperm out of the woman’s body, preventing fertilization | 96% with correct and consistent use | One of the least effective methods, because proper timing of withdrawal is often difficult to determine, leading to the risk of ejaculating while inside the vagina. | |
| 73% as commonly used (Trussell, 2009) | |||||
What if I am already pregnant?
Well no need to panic at all, Babies indeed are a blessing. Make sure to take good care of yourself and avoid stress. Reproductive Health Uganda clinics are open and you can visit at any working time, Monday- Saturday or better still, call ahead and set yourself an appointment with our well trained doctors.
Our prices are subsidised and are affordable. RHU boosts of over 60 years experience in providing quality and exceptional reproductive health services.

‘We’re not baby factories’: the refugees trying injectable contraceptives
‘We’re not baby factories’: the refugees trying injectable contraceptives- Article from the Guardian.com
Women who’ve fled South Sudan to Uganda are overcoming social stigma to explore new family planning options.

Christine Lamwaka fled South Sudan and now lives in the Palabek refugee settlement in Uganda. Photograph: Samuel Okiror
Christine Lamwaka and her husband gathered their six children and fled. It was April 2017 and their town in South Sudan had just been attacked. They walked for two days from Eastern Equatoria before crossing the border into Uganda.
“It was hard to flee with the young children. We struggled to run. I thought we couldn’t make it alive,” says Lamwaka, who was 22 at the time of the attack.
“We suffered a lot. I had given birth just a few months before and was breastfeeding. The children were crying. We are lucky to be alive.”
As well as ensuring her children were safe and the family had food and shelter, Lamwaka wanted to make sure she didn’t have any more children. But she was unable to access family planning services.
many children is very hard. We don’t have money for treating them, feeding and providing basic necessities,” says Lamwaka, from the safety of Palabek refugee settlement in Lamwo, northern Uganda. “We couldn’t afford to add more children.”
Research conducted by the Liverpool School of Tropical Medicine last year found that more than 40% of women in refugee settlements in northern Uganda who wanted to use contraceptives were unable to obtain them.
“Many health facilities in refugee camps are out or under-stocked,” said Simon Richard Mugenyi, advocacy and communications manager at Reproductive Health Uganda (RHU). Those seeking services often have to wait for organisations such as RHU to provide them.

South Sudanese refugees in the Palabek camp in Lamwo, northern Uganda. Photograph: James Akena/Reuters
Last year, however, Lamwaka enrolled in a pilot programme for a single-use, self-injectable contraceptive, Sayana Press. The contraceptive is being rolled out by the NGO Path Uganda, with support from the UN population fund (UNFPA), to promote increased uptake of family planning among refugees.”
In South Sudan, deep-rooted socio-cultural factors discourage family planning. The inevitable upshot is larger families. On average, women in South Sudan have 4.6 children. Among women aged 15 to 49 who are married or in a relationship, only 10% use any form of contraception. According to the UNFPA, this is the lowest rate in east and southern Africa, and many women have their first child while in their teens.
“I started giving birth while still a teenager. I was giving birth almost every year. There was no time to rest or for child spacing,” says Lamwaka.
“They need you to produce more children. Women are looked at as factories for babies. Men expect women to be producing a child every year.
“Women are not allowed to decide the number, timing and spacing of children.”
Uganda now hosts more than 1.3 million refugees, more than 850,000 of whom are from South Sudan.
About 75% of the more than 50,000 South Sudanese refugees at Palabek are women and children.
Lamwaka was pleased when she found out about the self-injectable contraception, which is taken every three months. It means she won’t have to seek out a health worker when she needs it, which is not always straightforward in a refugee camp.

Christine Lamwaka and her husband Solomon Olum decided that Christine should enrol in the Sayana Press programme. Photograph: Samuel Okiror
She and her husband, Solomon Olum, decided she should enrol in the programme. “We are struggling to raise these children. I don’t have a job. I am a farmer. But I don’t have enough land to farm here. I have to burn charcoal and do hard labour to get money to support the family,” says Olum.
More than 9,000 women began taking Sayana Press, a variation on the established contraceptive Depo-Provera, between April and November last year.
Edson Twesigye, a programme officer for Sayana Press, says the pilot scheme resulted in 43% more women accessing contraceptive services.
“This is a big achievement,” he says. “These are refugee women who had never used any family planning method in their lives because of cultural beliefs, lack of access, or other reasons. Reaching 43% is a great milestone.”
Julitta Onabanjo, the UNFPA regional director for east and southern Africa, says: “This is something we can take as a lesson learned as we look at how to introduce it into [our] programmes in other countries.”
Millions of women still don’t have access to contraceptives – report
There were social stigmas to overcome before the rollout of the new contraceptive, says Twesigye. His team had conversations with community and religious leaders, to position family planning “not as a way of stopping having children, as they thought, but as a way of planning how many children you want, when to have them and when to stop,” he explains.
He adds that men in village health teams in the area were also talking to other men to help them better understand family planning.
“Many women in these settings have a desire to plan their families and don’t have any method that suits them. Therefore being able to give them any option of [family planning] method is very important,” says Onabanjo.
Mugenyi says the Ugandan government must spend more on contraceptives, starting with the allocation of the $5m (£3.8m) it committed to provide each year at the family planning summit held in 2017.
“If the government honored this commitment, this would help to stock family planning commodities in public facilities, including those in refugee camps,” he says

RHU-Annual-Report 2015

RHU Annual Report2015
[pdf-embedder url=”https://www.rhu.or.ug/new-site/wp-content/uploads/2018/04/RHU-Annual-Report2015.pdf”]
